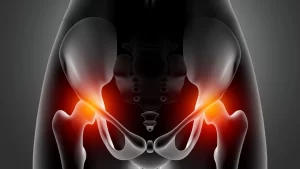
Hip Procedures
Hip pain refers to discomfort or pain in the hip joint, which is located where

Hip pain refers to discomfort or pain in the hip joint, which is located where
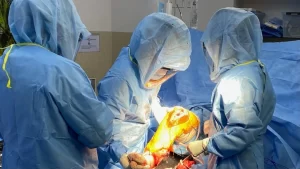
This simply means that only a part of the knee joint is replaced through a smaller incision than would normally be used for a total knee replacement. The knee join
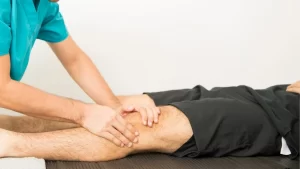
Non-surgical treatments are considered as a sub-speciality of orthopaedics which deal with all types of non-surgical treatments of orthopaedic and musculosk…


SMART knee replacement (only at our ortho hospital in Chennai), is a precise way of doing knee replacement surgery
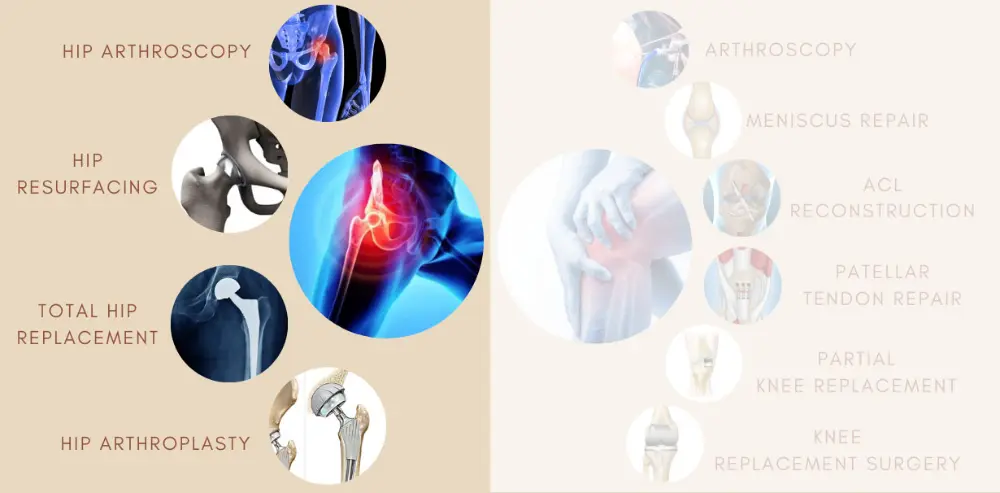
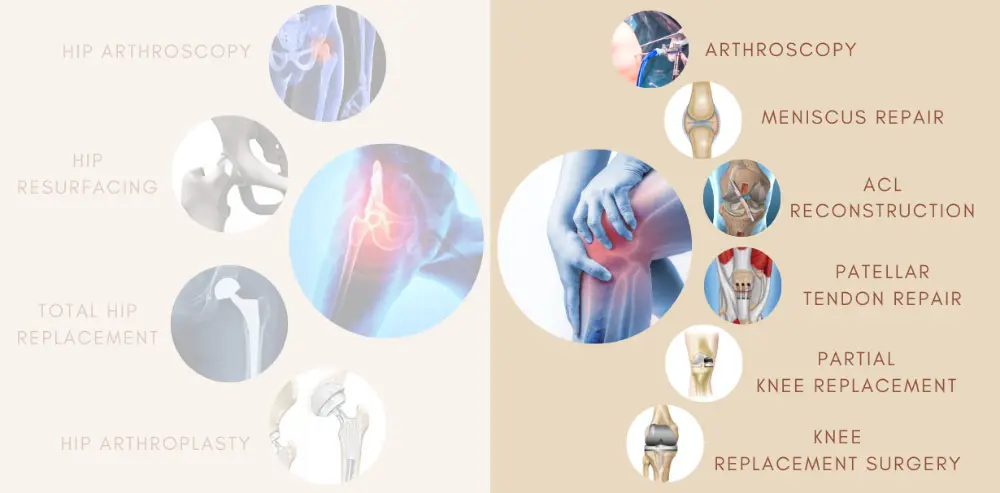
What makes us the best ortho hospital in Chennai.
A bit of our trusted reviews
After lot of suggestions and recommendations from my friends i visited Dr Bharath for my mom’s knee replacement surgery. He is so kind to boost confidence about the surgery and hear patience questions and respond to details. Surgery was done and my mom recovered in 2 months of time with no complications post surgery. Thank you Dr Bharath and his team.
I consulted Dr. Bharath for a problem with my knee. He made excellent diagnosis and took time to explain me things in detail. Encouraged me to undergo knee replacement surgery to solve the problem. His smart knee replacement technique enabled me to walk just after few hours of the surgery. He is a great professional and a very friendly person. I would definitely recommend him to anyone who needs a knee replacement.
Dr. L. Bharath is one of the most dedicated and efficient orthopedician in Chennai.His work was so perfect and my mother completely recovered from Hip replacement surgery without any complications.I strongly recommend Dr Bharath from VS hospital to have a safe and risk free joint replacement surgeries…
I would like to share my great personal experience with Dr Bharat. We met him exactly a month back on Aug.4th along with my Mother who was unable to walk (who had severe problems with both the Knees). Dr Bharat after reviewed my mother’s condition spoke very positive and sounded practical. He said we can go ahead with the surgery for the first Knee and within a week we can certainly proceed with the other knee. And in couple of weeks she can walk on her own without any issues. This was sounding like a dream to us. But actually he made it happen. Yes, my mother got the surgery done for one Knee on 11th August and the other Knee on 14th August. Both the surgery went on very well and my Mother has recovered very well. She is now started walking on her own without any support. Dr Bharat has made it happen for us. I really admire at his simplicity, humbleness and being passionate with his patients. I have no words to praise him. Whenever I called him, he was so polite and also precise to the point showing utmost care, love and affection.. He gives the entire credit to his team and yes it is a fantastic Team Work with utmost dedication. My personal thanks to Dr Bharath who has made our dream come true by preparing my mother to walk on her own. Thank you sir once again for you and your great Team. At this juncture I also want to thank our Family Doctor, Dr. Zia Ullah Khan, Chennai who referred us and guided us to Dr Bharat. Thank you sir. I really feel proud and happy to share my honest feedback and I am keen to share your details and recommend it to all my contacts who can benefit through your wonderful service. God bless you and your Family sir 🙏
Five start will never be enough for such a wonderful doctor. Really thanking DR. Bharath for the successful surgery for my 80+ grandmother. She is walking now very happily and feeling the confidence back in her. Thank you sir for it. I really wanted to thank sister Keerthana for taking care of my grandmother like her own relation and she became one of the member in our house now. Thank you both for making my grandmother to walk again and if I look back and see what I achieved in my life. This will be one of my memory in seeing the smile in my grandmother’s face. Thank you Bharath sir and Keerthana akka
We were also impressed with the clear communication and thorough explanations provided by the doctor and his team throughout the entire process. They took the time to answer all of our questions and concerns, and we felt fully supported throughout.
Thank you again for your excellent service and care!
Had knee replacement surgery done by him, 2 weeks post op I’m completely pain free now, I’m able to do my routine works now and doing all my physio exercise normally. Thanks to Dr. Bharath’s expertise and techniques, my surgery was very successful.
Dr. L. Bharath did a wonderful knee surgery for my father and provided great care from start to finish. During the pre consultation, he was very informative and specific and guided us in the right direction. He also provided wonderful care post-op and made my father feel comfortable after the surgery. His team provided personalized care and continue to clarify our questions, even a month after the surgery. I would highly recommend Dr. L. Bharath and his team for anyone considering to get a knee replacement.
My mother was suffering with alot of pain in her knees she was not able to walk so we tried all sort of therapy for her but nothing worked and then we were referred to Dr. L. Bharath who then explained clearly to us about the joint replacement surgery and did the surgery for my Mother which was successful. It’s been 56 days now and my Mother is just doing great she’s able to walk she’s able to climb the stairs and she’s able to do things by herself A very big Thank You to Dr. L. Bharath who treated us like family and talked very politely and made this surgery a big success for my Mother we are all very happy that my mother is back and up on her feet.
Thank you for all the care that you have given for my father. You have made sure that he was always given the best care available. Your compassionate attention and professional care made us feel safe. There are not enough words for us to express our appreciation. Because of your excellent care my father able to walk without pain. Keerthana’s sister’s service and care is much appreciated.
Dr. L. Bharat is very friendly, skillful and a caring doctor. He treats his patients as his family member.Iam flabbergasted to see my mom walking a few steps on the very next day of knee replacement surgery .It is because of the experience of Bharat sir in knee replacement surgery. Keerthana sister is service minded and caring.My gratitude and regards to the whole team.
After visiting few doctors for my mother’s knee replacement surgery I had found Dr. L. Bharath the best among them. He had given the best treatment and the recovery of my mother was also so smooth, most importantly he had given us a detailed explanation about the operation and its recovery which gave me the confidence to proceed. Also how many ever times you ask him doubt he will explain without any hesitation and his assistant (Keerthana) also gave us the best support. I had also heard about his previous surgery and its success rates yet again he proved it in my mother’s surgery. After 15 long years I am seeing my mother walk straight without any knee pain or any kind of support. If you ever have any orthopaedic issues without any doubt he will be the best option to get the relevant and perfect treatment.
My mother-in-law underwent knee replacement surgery last week, entire process went on with a ease. With limited support from family and unlimited support from Doctor and VS Hospital staff this was successful.. Would like to thank you and definitely recommend Dr. L. Bharath for others.
I was suffering with chronic knee pain and my left leg got slightly curved/bent. One of my friends who also had knee problem on both his knees shared the wonderful experience he had with Dr.Bharath and his expert team. Based on his recommendation and highly satisfactory knee surgery result, I approached Dr.Bharath and after the first initial assessment he said that my knee problem is nothing major to be worried and can be easily remediated with a simple surgery. He educated me with adequate information about the surgery procedure and benefits of knee surgery. That gave me great confidence and motivation to proceed with the surgery. Thereafter his team including Dr.Keerthana showed good cooperation and support to get rest of the medical tests done, which assured me of their high service standards. I found Dr.Bharath to be very kind, supportive and positive in his approach and at the same time not very pushy. He gave me sufficient time to make my decision regarding surgery and provided with all required information such as surgery benefits, pre and post-surgery care and recovery procedure. I truly appreciate his passion and approachable nature. If not for the doctor and his team, I don’t think I would have gone ahead with my surgery. I got admitted in the hospital one day before surgery and pre-surgery care was excellent. My son also stayed with me in the hospital to provide moral support. Surgery was done in 1 hrs time on 10th Oct and they took care of me very well, right from food, medicine, daily personal routines and physio practice from day 1 after surgery. I was discharged from hospital on 4th day and here I am happily sharing my experience. I would strongly recommend people with knee problem to approach Dr.Bharath’s hospital for advice and medical care.
Hi, I would like to thank you from the bottom of my heart for giving me my mom’s life back. Before seeing you her activities were extremely limited. She was struggling with the leg pain over the past 15yrs and so both the knees were damaged to the extreme stage.
Dr. Bharath Believe me your services will be highly recommended to all that I know. You made our dream come true.
I still can’t believe that the pain and healing time were so minimal and that she was walking long distance on her own within only a few weeks of the procedure. I am so pleased that she can now function without any pain or limitations. Thanks to you and your team.
My father underwent total knee replacement surgery on 17/06/2022 and 20/06/2022 by Dr. Bharath at VS Hospitals. The entire process was extremely friendly and easy both on the patient as well as on the family members. Dr. Bharath is very professional, transparent, friendly and down to earth person who took utmost care of my father every single day during our stay at the hospital. He explained every single doubt about the surgery and was easy to approach any time of the day which typically might not be possible with all doctors. My father was made to walk on the same day after about a few hours of the surgery with the help of walkers which was incredible. He was able to walk without walker support the second day of the surgery and became completely independent at home after getting discharged from the hospital. The smart surgical procedure conducted by the doctor was very helpful especially for the post surgery recovery and pain management. Keerthana sister was very caring and helpful through the process. We would definitely recommend Dr. Bharath to all our family and friends network. We pray God to bless the doctor and his team abundantly so that a lot more people can get benefitted out of his expertise. Thank you!


Orthopaedic Surgeon
Dr. L Bharath is one of the leading orthopaedic surgeons in Chennai and the founder of Bharath Orthopaedics. Dr. L Bharath specializes in Knee & Hip surgery includes primary, complex & revision (previously failed) joint replacements, sports injuries & arthroscopic (keyhole) procedures. Having performed over 10000 surgeries with a phenomenal success rate, Dr. L Bharath stands out as among the best orthopaedic surgeons in India (& the best orthopaedician in Chennai ) with his extensive focus on upgrading himself on procedures and operations, in particular, the Joint replacement surgery.

Knee pain is common and is not always a sign of anything serious. It can be due to many possible causes which include simple….

In today’s medical era, one of the most common orthopaedic
Mon-Sat 9 am to 8 pm | Sun – 10 am to 3 pm
© 2024 All rights reserved |⚡ by Cloudstar Digital